Meet Pam

I am an advocate and a metastatic breast cancer thriver. I am telling my story because a PET scan likely prolonged my life.
In 2010, I was treated for Stage 1 estrogen-positive breast cancer. My prognosis was good because I had a small tumor with no lymph node involvement. Seven years later my physician diagnosed a local recurrence of the original breast cancer. To be certain it was a local recurrence, I advocated for a PET/CT scan. Unfortunately, I was right: the scan confirmed the disease was not local and I received the hard and scary diagnosis of Stage IV metastatic breast cancer. If I had not asked for that PET/CT scan, my disease would have been staged incorrectly, and I may not be telling this story now.
I am sure that this early and proper diagnosis is why my disease remains relatively stable and I have been able to stay on my first line of treatment.
As a cancer patient, I know the importance of getting nuclear medicine procedures right. For years, I have had a PET/CT scan every 12 weeks. Getting the image right matters to my treatment plan and my life. An improper radiopharmaceutical injection that puts some radiation in my tissue instead of all of it in the vein can lead to unnecessary radiation exposure and compromise the images that I need to be right. I know my caregivers try their best, but I also know that extravasated injections can happen, and my physicians can be unaware the image has been compromised.
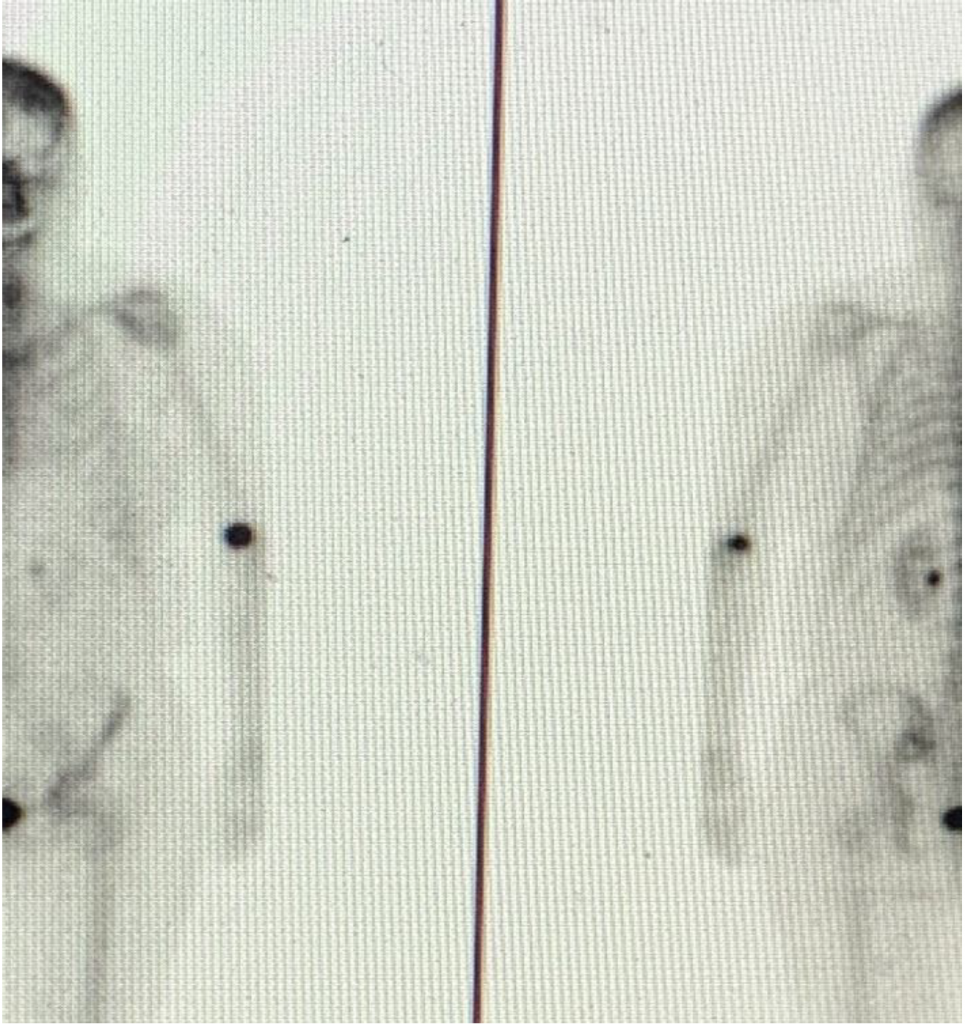
Learn more here.
I also know that today, nuclear medicine injections are not monitored. They are not monitored because the Nuclear Regulatory Commission implemented a policy in 1980 that exempts ALL extravasations, no matter how severe they are, from being reported to the NRC. This also means that hospitals do not have to tell patients. Patients and doctors need to know when a patient has been unintentionally exposed to a large radiation dose that can also compromise their images or treatment.
Hospitals need to know if they are accidentally putting patients at risk and they need to be transparent regarding their nuclear medicine injection quality, so patients can choose centers with the highest quality images for their care.
Pam
My Public Comments to the Nuclear Regulatory Commission
- August 30, 2021 – I was extravasated and my clinical team did not know what to do.
- July 11, 2021 – Questions for nuclear medicine centers about how they monitor for extravasations.
- November 27, 2020 – The extravasation reporting exemption must go.








